The definitions below roughly follow the order of appearance in the story and are organized by chapter. Most of our medical and surgical terminology derives from Greek or Latin, so anything that is italicized originated from one of those two languages. WARNING: there are a handful of rather graphic photos, so proceed with caution.
CHAPTER 1
Steam stacks: If you live in New York City (and probably other northern cities), you will be familiar with these. There is a system of steam pipes under the streets, and if they rupture, steam stacks are used to divert the steam away from street level.

Black curtains: Patients who have lost consciousness due to heart attack, cardiac arrhythmia, or severe blood loss (Michael Smith, who is bleeding internally), often describe the sensation, if they live to describe it, as black curtains lowering over the eyes.
CHAPTER 2
Agonal: Agony is defined as intense pain of mind or body, or the struggle that precedes death. Agonal respirations are feeble gasps of air that are insufficient to sustain life. Immediate intubation is paramount.
Airway: The nose, mouth, pharynx, larynx, and trachea all comprise the airway—the path that air follows from the atmosphere to the lungs. Maintaining “control” of the airway is the first priority when treating a severely injured trauma patient.
Larynx: the “voice box” or “Adam’s apple.” This is where the vocal cords reside and the trachea begins.
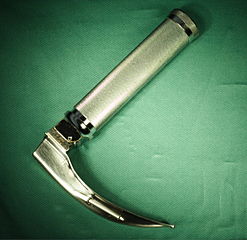
Laryngoscope: an L-shaped instrument with a handle and a detachable blade. The blade is placed into the pharynx, and by lifting the base of the tongue, the vocal cords (which reside in the larynx) are visualized. The endotracheal tube is then advanced through the cords into the trachea.
Endotracheal tube: a plastic tube that is inserted through the mouth (or nose) and advanced into (endo = within) the trachea. It gives the first responder or ER physician control of the airway.
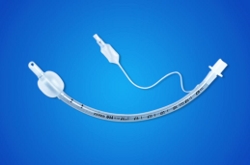
Intubate: the act of placing an endotracheal tube.
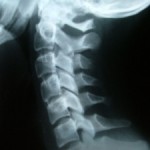
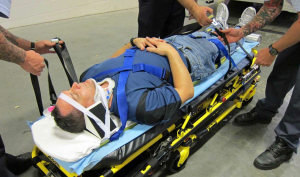
C-collar: a rigid collar used by first responders to stabilize the cervical (neck) spine until x-rays can be obtained to rule out injury.
Backboard spinal stabilization: In an unresponsive trauma patient, the first responders have to assume spinal injury is present until proven otherwise. For this reason, the full length of the spine–cervical, thoracic, and lumbar–is fully immobilized prior to transport. Patients that are still unresponsive upon arrival at the emergency department remain on the board until a full series of spinal x-rays are completed and spinal injury is ruled out.
Ambu or oxygen bag: a pliable plastic bag the size and shape of a football. By repeatedly squeezing the bag, oxygen is pumped into the lungs. During respiratory distress or cardiac arrest, bagging is preferred over mechanical ventilation in that a higher respiratory rate can be achieved.
Feculent: foul with impurities, but most often associated with the properties of feces (stool; excrement). For example: a feculent odor, a feculent discharge, hair matted with feculent material, etc.
“Give report”: Every writing teacher, workshop student, and editor who has critiqued my manuscript has tried to get me to add “his” to the line “Burnett waited to give report,” as in “give his report.” Give report is jargon used by nurses, physicians, students, first responders, and anyone else relaying patient information to another caregiver.
Ventricular fibrillation: complete loss of the rhythmic contraction of the heart. The muscle fibers continue to contract, but in a disorganized and independent fashion, giving the fibrillating heart a “bag of worms” appearance. No longer receiving blood, the heart muscle quickly becomes hypoxic (hypo = under; ox- = oxygen) and turns a blackish-blue color. Without treatment, VF is fatal within minutes.
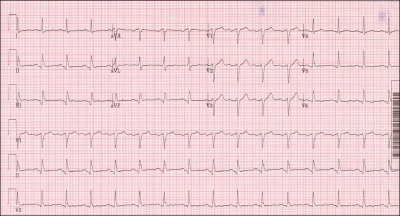
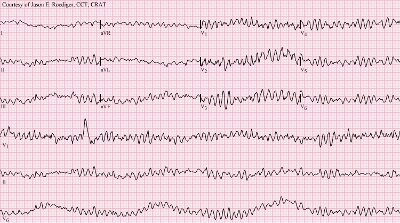
Epinephrine: one of the stress hormones. Secreted by the adrenal glands, it is also known as adrenaline. Epinephrine and its cousin norepinephrine stimulate the heart to beat faster and more forcefully, and quickly raise the blood pressure by constricting the arterial system. During cardiopulmonary resuscitation (CPR), pharmaceutical epinephrine is given IV push.
IV push: A medication is given intravenously using a syringe.
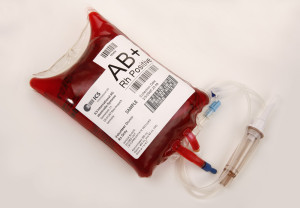
O-negative: The O-negative blood type is the universal donor. Because O-negative red blood cells lack surface antigens, they do not initiate an immune response and can therefore be transfused into a recipient of any blood type. When resuscitating a crashing trauma patient who is clearly bleeding, you can’t wait for the lab to run a type and crossmatch, so you transfuse units of O-negative until the type and cross is completed.
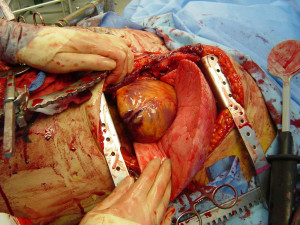
“Let’s crack him”: The ER thoracotomy–in my opinion, this is the most dramatic procedure in all of medicine and surgery. Thoraco- derives from the Greek word thorax (chest), and -tomy comes from the Greek word tome (incision), so thoracotomy is the surgical term for incising the chest. “Cracking” a chest is jargon for a thoracotomy performed in the emergency room. Read my blog post for a thorough discussion of this topic, and to view some graphic (and possibly disturbing) videos of actual ER thoracotomies being performed. If you’ll go to part 3 of the Me, Myself and I interview, I’ll share my experiences with this procedure and describe the first ER thoracotomy I performed, which was quite dramatic, even by ER thoracotomy standards.
Rib spreader: a heavy retractor that generates significant leverage, thus allowing the ribs to be spread apart far enough to allow access to the chest cavity.

Cross-clamp: Vascular clamps come in a variety of shapes and sizes. A long, slender clamp is necessary to reach deep in the chest and cross clamp (totally occlude) the aorta.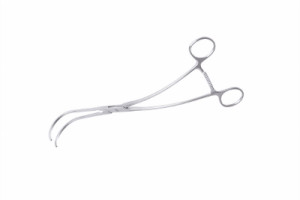
Internal paddles: small defibrillator paddles that can fit inside the chest. The electrical current is delivered directly to the heart, thus resulting in a greater chance of defibrillating the heart and restoring a rhythm capable of pumping blood.
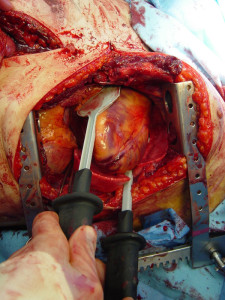
Kidney resection: Resectus is Latin for cut off, or cut out, a portion of a structure or organ. Thus, removal of a kidney.
CHAPTER 5
Laryngectomy: ectomy is the complete removal of an organ. Thus, removal of the larynx.
“Monkey-faced people”: Alzheimer’s disease is a real scourge. My mother had it, and paranoia was a prominent feature, as it is for many patients. Within the first year of her diagnosis she was seeing chicken-faced and monkey-faced people wandering the halls of her assisted care facility. Sometimes they would follow her around and threaten her. At other times they would pop up through the floor of her room and frighten her. They made her existence quite difficult, and then one day they just disappeared. If someone close to you is suffering from this disease, my heart goes out to you.
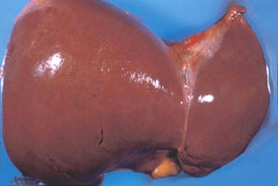
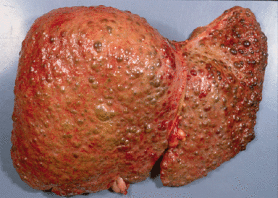
Cirrhotic: (sĭ-rŏt´ik) the adjective of cirrhosis (sĭ-rō´sĭs). Cirrhosis is a chronic disease characterized by degeneration and scarring of the liver. If enough healthy tissue is replaced by scar, liver failure occurs and transplantation is the only option for survival.
CHAPTER 7
Lebsche sternal knife: In the early days of cardiac surgery (the late 1950s and early 1960s), the Lebsche knife was used to open the sternum. The little nub on the bottom, the foot plate, was hooked under the edge of the sternum, and a mallet was used to drive the knife blade lengthwise up the middle of the sternum. The Lebsche knife was eventually replaced by pneumatic powered saws but is still used today to rapidly divide the sternum during emergency room thoracotomy. For the ER thoracotomy, an incision is made on the left side of the chest from sternum to scapula, but most often, the sternum needs to be divided in half in order to enlarge the incision and provide greater exposure. Three or four swings of the mallet will generally get the job done.


CHAPTER 14
Extracellular: extra is a prefix meaning outside of, in addition to, or beyond. Extracellular means outside of, or beyond the cell wall.
Porcine scaffold: The use of mammalian organ scaffolds, primarily ferret and porcine (pig), is an area of great promise in the effort to grow bioengineered human organs in the laboratory. The intact animal organ is placed in a detergent bath of Triton X-100 and ammonium hydroxide, which washes away all the cellular components, leaving behind an extracellular matrix of non-immunogenic proteins and polysaccharides (complex, structural sugars). This de-cellularized matrix is then infused with progenitor cells (a close descendant of the stem cell) and endothelial cells (which form the lining of blood vessels and other tubular structures within organs). By using a scaffold that has been “cleaned” of all “donor” cellular components, and infused with the recipients own progenitor and endothelial cells, the bioengineered organ will not trigger an immune response when transplanted into the human recipient.
Histology: the microscopic study of tissues. Cells form tissues. Tissues comprise organs. A collection of organs make up an organ system (the cardiovascular system, for example). Organisms are a collection of organ systems.
Necrotic: dead, but specifically, an area of dead tissue bordering, or surrounded by, viable (living) tissue.
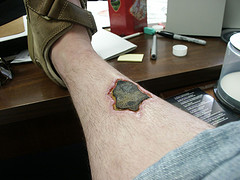
(Jeffrey Rowland flickr/unaltered)
Ischemic injury: Ischemia (is-kē’-mē-ə) is the loss of blood flow to a tissue or organ. Ischemic injury occurs when the lack of blood flow is prolonged to a sufficient extent to result in tissue injury. If ischemia persists and results in cell death within an organ, the dead area represents an infarct. Thus, a myocardial infarction (heart attack) is the end result of obstruction of a coronary artery, resulting in ischemic injury and subsequent death of an area of myocardium (myo = muscle; kardia = heart ).
Arterioles, venules, capillaries: the smallest divisions of the vascular tree. As arteries branch, they become progressively smaller. Arterioles are the smallest branches of the arterial side of the vascular tree. Venules are the smallest of the veins. The capillaries connect the two. Blood flows through the arterioles into the capillary bed. Nutrients and oxygen are exchanged for carbon dioxide and waste products. The venules carry the deoxygenated blood into the veins and back to the lungs.
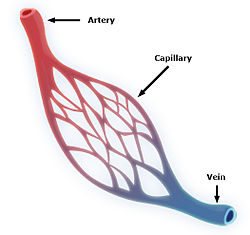
Vascular: pertaining to the blood vessels of the body. A vascular clamp is used to temporarily obstruct the flow of an artery or vein. A vascular surgeon specializes in the surgical treatment of arterial and venous injuries and diseases.
Perfusate: a fluid or solution that is perfused, or forced to flow through, an organ or tissue.
Anaerobe: a microorganism that thrives best or lives exclusively in the absence of oxygen.
Pathophysiology: pathos is Greek for disease. Pathophysiology, then, pertains to the physiology of an abnormal state, or more specifically, the functional changes that accompany a particular syndrome or disease.
CHAPTER 15
Intracellular: intra means within, so intracellular means within a cell.
Protein Synthesis: the formation of proteins from amino acids.
Lymphatics: pertaining to the lymph vessels. Fluids exuded from the blood vessels into the tissues are gathered up and carried back to the bloodstream via the lymph vessels.
CHAPTER 16
Temporary Colostomy: an ostomy is a surgically formed opening that is frequently temporary but may be permanent. A colostomy is a connection between the colon and the abdominal wall. Following the surgical repair of penetrating trauma, such as a gunshot or stab wound to the colon, a temporary colostomy will be formed upstream of the injury to divert the fecal flow away from the repair, thus giving the wounds a chance to seal themselves and heal.
CHAPTER 17
The Surgical Team: The surgical team generally consists of a surgeon, a surgical assistant, a scrub nurse, a circulating nurse, and an anesthesiologist. Depending on the complexity of the case, there may two assistants, scrub nurses, circulators, etc. Or, for a small case, the scrub nurse may also function as the assistant, or a surgical assistant might not be used at all.
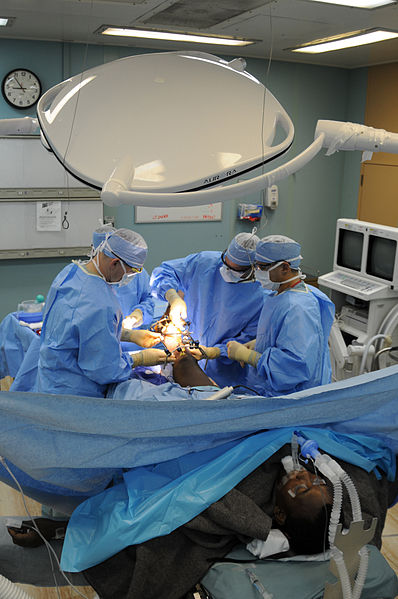 The Sterile field: Contrary to popular belief, the operating room in not a sterile environment. The operative field, however, is sterile and is defined by sterile drapes, the sheet separating the field from the anesthesiologist, and the personnel at the table. The surgeon, scrub nurse and assistants are considered sterile from waist to shoulders, so their hands must not be raised or lowered above or below those boundaries.
The Sterile field: Contrary to popular belief, the operating room in not a sterile environment. The operative field, however, is sterile and is defined by sterile drapes, the sheet separating the field from the anesthesiologist, and the personnel at the table. The surgeon, scrub nurse and assistants are considered sterile from waist to shoulders, so their hands must not be raised or lowered above or below those boundaries.
If the surgeon’s nose itches, the circulator (who does not maintain sterility) will scratch it through the mask. If the scrub nurse needs additional supplies or instruments, the circulator will retrieve them and drop them onto the instrument tray or back table using sterile technique, and so on. Once the surgical wound is closed and dressed, the sterile field is irrelevant and everyone can remove their gowns and gloves.
Mayo Stand: a smallish instrument tray that can be positioned over the patient, adjacent to the operative field.

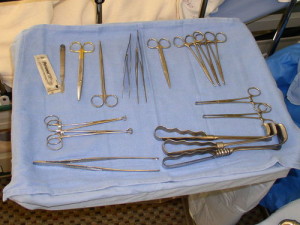
The majority of the instruments, supplies, and other equipment are kept on the back table and moved to the Mayo stand as needed.
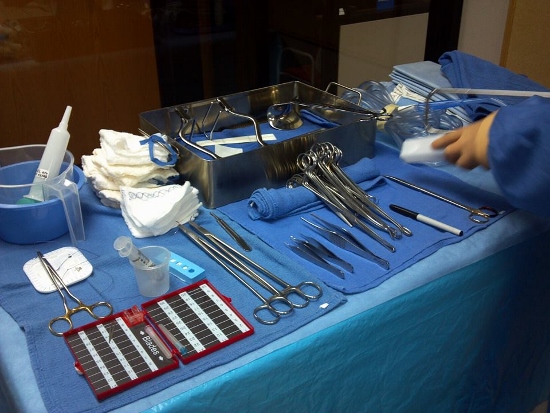
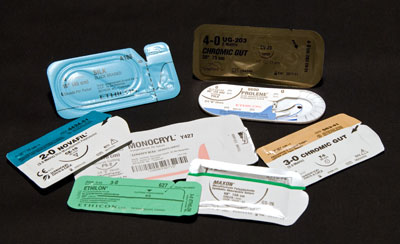
Suture Packs: packages of sutures. Some sutures are made of natural material, like silk or catgut (chromic gut in the photo), and some are synthetic (Prolene, Monocryl, Novafil).
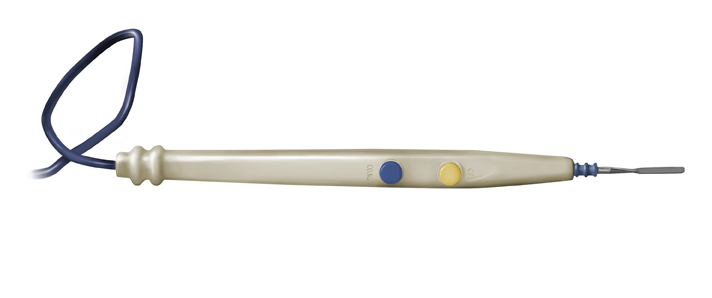
Electrocautery Device: the electric scalpel. In cut mode this baby slices through tissues like warm butter, but the tissues bleed like crazy. In coag, or coagulate mode, the current is more diffuse, thus coagulating the capillaries and small blood vessels as the tissue is divided. In a highly vascular tissue like muscle, the cautery device is not only an invaluable time saver, but it greatly reduces blood loss.
Anesthesia Cart: also known as the anesthesia machine. The cart is home to the ventilator (note the corrugated tubing and mask), the atomizer that delivers the inhalational anesthetic agent, multiple monitoring devices, and drawers full of drugs that Tyronne Pradeaux and his crew would kill for.

CHAPTER 18
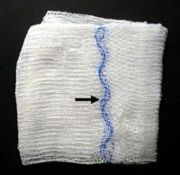
Ray-Tec sponges: the trademarked name for x-ray detectable sponges. These highly absorbent 4″ x 4″ sponges have a radiopaque lead filament sewn into them. If the sponge count isn’t correct at the end of the case, an abdominal x-ray is performed before the patient is taken off the table. If the missing sponge is in the abdomen, the wound is reopened and the sponge is removed before the patient is awakened from anesthesia and transported to the recovery room.
Midaxillary line: Axilla is the anatomical term for the armpit. Draw a straight line from the center of the armpit down to the brim of the pelvis, and that is the midaxillary line.
Fascia: (făsh′ i-ŭ) a connective tissue sheath that joins the skin to underlying tissues. It also surrounds and separates muscles and muscle groups.
Laparotomy sponges: Also known as lap sponges, they resemble small towels and possess great absorbency. Ideal for soaking up blood, pus, and other fluids.

Forceps: medical term for tweezers or pincers. DeBakey forceps (pictured below) were specifically designed by cardiovascular surgery pioneer Michael DeBakey to minimize trauma to the tissues being grasped, particularly the vascular structures.

Reapproximate: suturing together surgically divided tissue layers.
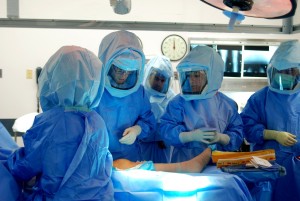
Hooded surgical gowns: Used primarily by orthopedic surgeons during joint replacement surgery, these specialized gowns offer added protection against postoperative wound infection, which can be devastating in a surgically replaced joint.
CHAPTER 20
Old Bellevue Psych Hospital: As a cardiothoracic resident in the NYU system, I often travelled by foot from NYU Medical Center to Bellevue Hospital, which was a couple of blocks down Third Avenue from NYU. Late in the afternoons I often encountered a long line of homeless men and women in front of the original Bellevue psychiatric hospital. One day I asked them why they lined up there every afternoon, and they told me that after the psych service moved into the new hospital they began using some of the wards of the old hospital as a homeless shelter, but space was limited, and it was a first come, first served system. That was back in the early 1990s. I don’t know if this still happens.


CHAPTERS 21 – 40: Go here.